Click on the link below to access a variety of forms
Horse Health Free Reports

Click on the link below to access a variety of forms
Horse Health Free Reports
Learn equine biosecurity basics for the farm, horse show, and breeding shed to protect your horses from infectious diseases.
— Read on thehorse.com/features/practical-biosecurity-tips-to-protect-your-horse/
Learn about the diseases veterinarians recommend protecting your horse against and how vaccination could save your horse’s life.
— Read on thehorse.com/features/core-vaccination-protecting-horses-from-5-deadly-diseases/

I have been using the app “HorseNotes” on my iPhone for over a year. It is by far the best software I have ever used and the best part is…you can access it on your computer as well as your iPhone (I believe it is also available for other smartphones).
Horsenotes.co allows me to make a profile for each of my horses and track their health, shoeing, tack, feed, vaccinations, worming, everything….There is a note section where I am able to log what I did that day with my horse. I can log everything I purchase or every horse-related expense and with a press of a button the app/website even generates an expense report. I can keep all of my contacts in one place- vets, stables, farriers, tack stores, etc. The app has a calendar that alerts you when you need to book the farrier or when the vet is coming. Plus, I can provide a log in for other people to add information as well. You can upload records (sales, purchases, competition info, coggins) and pictures as well. Seriously, I don’t know how I was able to keep track of everything before I began using this incredible app!

I had the vet run some blood work on Luck and Chance as a precaution, because of the “Panic Grass” in Virginia has been causing liver failure in horses, and because I like to do a full work up every 6-12 months.
Chance’s Blood Work

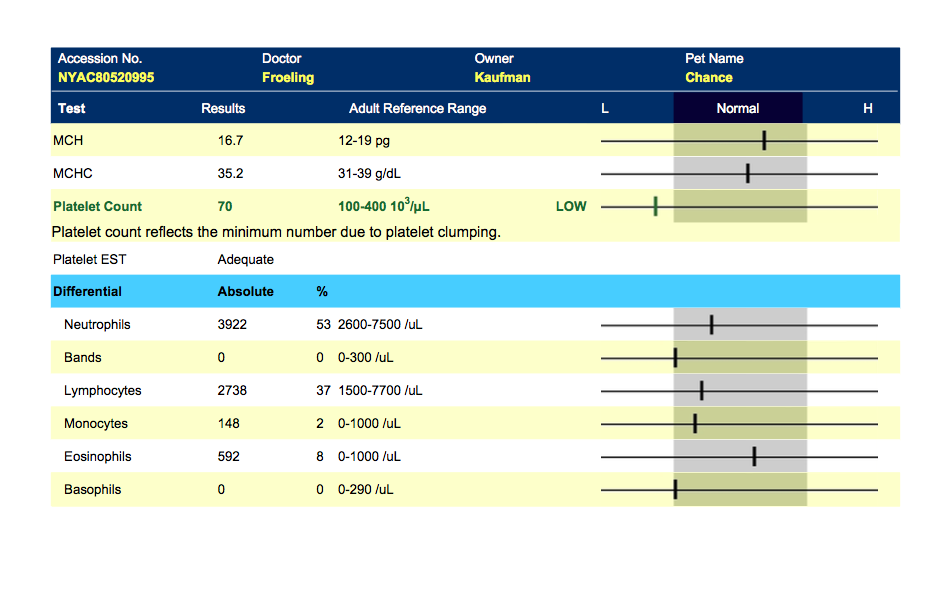

INTERPRETATION OF RESULTS
Elevated Potassium (6.6 mEq/L):
Low Sodium:
“Low levels commonly indicate loss through excessive sweating, or through kidney or intestinal disease. Low levels may also be found in young foals with bladder damage. Increased sodium levels are usually a sign of dehydration” (http://www.minstervets.co.uk).
Low Platelets:
This was the most worrisome in regards to the potential immediate issues that could ensue because of the low platelet count.
Low Glucose:
“Glucose is the source of the body’s energy. It is measured in suspected cases of equine metabolic syndrome and sometimes in cases of equine Cushing’s disease. Blood glucose may also be measured as part of a glucose tolerance test, assessing small intestinal function” (http://www.minstervets.co.uk).
Levels 2-3x the highest number in range are considered significant according to vetstream.com. Levels are easily increased due to poor handling techniques as well as lab error.
According to Dr. Christine Woodford and Carla Baumgartner on vipsvet.com, “Elevations of CPK and SGOT are indictors of muscle inflammation–tying-up or rhabdomyolysis. The term “rhabdo” means muscle and “myolysis” means rupture of muscle cells. The CPK and SGOT are very sensitive indicators of skeletal muscle damage, and they rise in concentration proportionally with the amount of damage. A bit of timing is required in order to obtain the most sensitive results; CPK rises (due to its leakage from muscle cells into the blood system) approximately six to eight hours after the onset of muscle inflammation, and SGOT rises after approximately 12-14 hours. The absolute peak of CPK concentration and the time it takes to return to normal are important indicators of the severity of muscle damage and the response to therapy.”
Elevated MCV: Is the average volume of red blood cells.
According to Vetstream.com, “Macrocytosis (increased MCV) resulting from release of immature RBC from the bone marrow during regeneration is very rare in the horse therefore the MCV is less useful in the horse than in other species.”
Elevated MCH: Is the average amount of hemoglobin in an individual red blood cell.
Low RBC:
Luck’s blood work

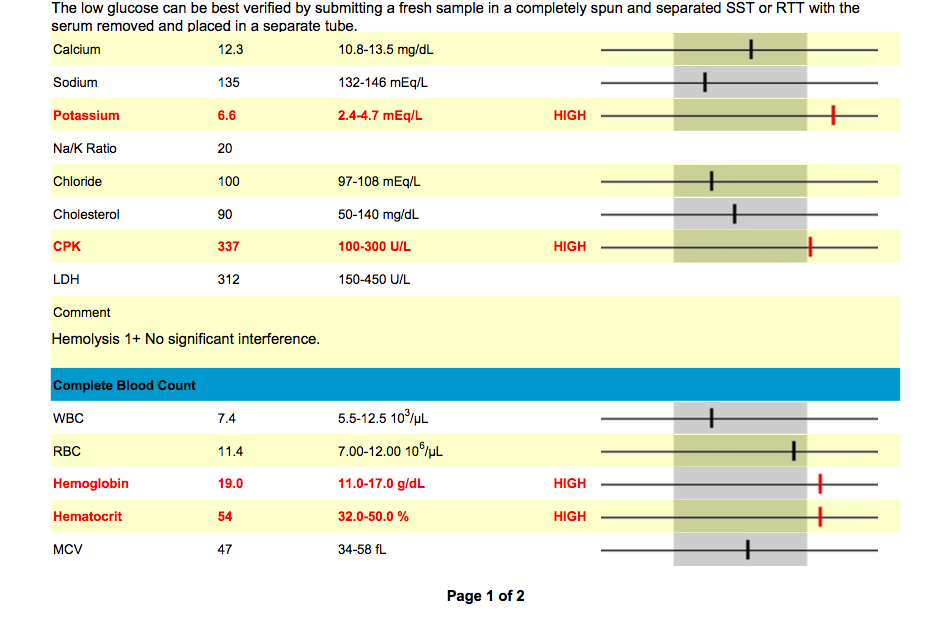
Elevated Potassium: Potassium can become elevated for a number of reasons.
According to Vetstream.com,
In combination with clinical signs and results of other tests results could signify the following;
Elevated GGTP:
* Donkeys tend to have 3x higher levels then horses. This means that in stead of the typical equine range being 1-35 U/L a typically donkey’s range would be up to ~105 U/L. Lucky’s test showed he had 120 U/L which is still elevated but not much. It took sometime to get Luck from the field when the vet arrived- he ran around non stop. The excitement and anxiety could be the cause of the elevated levels.
RBC:
Katherine Wilson, DVM, DACVIM, of the Virginia–Maryland Regional College of Veterinary Medicine (See more at: http://equusmagazine.com/article/decode-horses-bloodwork-27122#sthash.sc4J1ISJ.dpuf) explains “RBC count is probably the least helpful information because horses usually don’t have big changes in red blood cell numbers. It is not uncommon for horses to have an RBC count a little lower than normal range, however. The term we use for low RBC is anemia, but unless the count gets very low, a horse doesn’t necessarily need to be treated for that condition. A lot of diseases or any chronic long-term disease can cause mild anemia. Usually if we see mild anemia on the bloodwork and the horse has other issues, the anemia is just an indication that we need to fix/treat another problem.”
Low or Elevated Values
Low Bilirubin:
Elevated Hemoglobin (19 g/dL):
According to vetstream.com, Thoroughbred and other “hot-blooded” horses Hemoglobin range differs from other equine- the thoroughbred range = 11.0-19.0g/l.
Elevated Hematocrit (54 %):
Elevated levels could be due to;
“A measurement of the relative amount of red blood cells present in a blood
sample. After blood is drawn, a small tube is filled and centrifuged to separate the heavier
blood cells from the lighter white blood cells and the even lighter fluid (plasma or serum)
portion. A higher than normal reading generally indicates dehydration (same number of
cells in less plasma volume) or may be due to splenic contraction secondary to
excitement or the demands of exercise. A low reading may indicate anemia, though not
invariably. Highly fit athletic horses may normally have a slightly lower hematocrit at
rest due to an overall more efficient cardiovascular system. Evaluation of true anemia in
horses requires several blood samples over a 24-hour period” (Susan Garlinghouse, 2000/ http://www.equinedoc.com/PrideProjectInfo.html).
It took sometime to get Luck from the field when the vet arrived- he ran around non stop. The excitement and anxiety could be the cause of the elevated levels.
Low Sodium:
According to horseprerace.com, “Low levels indicate depletion and are often a predisposing factor, along with dehydration, in fatigue, muscle cramps, colic, synchronous diaphragmatic flutter (“thumps”), diarrhea and other symptoms of exhausted horse syndrome. Even seemingly normal or high-normal levels may in reality be lower, but appear higher due to concentration secondary to dehydration as measured by total protein and albumin levels. Therefore, levels at the lower end of the normal range should be evaluated relative to concurrent dehydration.”
More information on your horse’s blood work
Decoding your horse’s blood work
A Better Understanding of the Results
The vet suggested that I add water to Luck’s and C’s feed in case their values are due to dehydration. She also explained that some of the values may be a result of running around in the field right before drawing them along with anxiety.
The anxiety and running around seemed fair but I am hesitant on the dehydration portion. Yes, I know it is winter and that horses are less likely to drink as much water. But if it were due to dehydration then the Albumin would be low as well. But, the blood work revealed that the Albumin was 2.8 (Luck) and 3.2 (Chance). These values are within the normal range…. that being said, the results could also be due to lab handling especially the Potassium levels.
While speaking with my uncle Jerry (the horse whisperer), he suggested adding a salt block to the horse’s feed. This will increase the horse’s thirst which will get them drinking more. I also added heated water buckets so that the water won’t freeze and in case they are less inclined to drink when the water is cold.
In order to feel comfortable about my horse and donkey being healthy, I will have more blood work done this week to make sure everything is in fact okay.

You don’t want to waste time in an equine emergency! The American Association of Equine Practitioners (AAEP) offers these tips to keep you organized and calm in your horse’s time of need.
If you own horses long enough, sooner or later you are likely to confront a medical emergency. From lacerations to colic to foaling difficulties, there are many emergencies that a horse owner may encounter. You must know how to recognize serious problems and respond promptly, taking appropriate action while awaiting the arrival of your veterinarian.
Preparation is vital when confronted with a medical emergency. No matter the situation you may face, mentally rehearse the steps you will take to avoid letting panic take control. Follow these guidelines from the American Association of Equine Practitioners (AAEP) to help you prepare for an equine emergency:
Many accidents can be prevented by taking the time to evaluate your horse’s environment and removing potential hazards. Mentally rehearse your emergency action plan. In an emergency, time is critical. Don’t be concerned with overreacting or annoying your veterinarian. By acting quickly and promptly, you can minimize the consequences of an injury or illness.
For more information about emergency care, ask your equine veterinarian for the “Emergency Care” brochure, provided by the AAEP in partnership with Bayer Corporation, Animal Health. More information can also be obtained by visiting the AAEP’s horse health web site, www.myHorseMatters.com.
The American Association of Equine Practitioners, headquartered in Lexington, Kentucky, was founded in 1954 as a non-profit organization dedicated to the health and welfare of the horse.
– See more at: http://practicalhorsemanmag.com/article/eqemergenc2576#sthash.YFzhhSOX.dpuf

 The month passed by slowly….I kept hitting a brick wall over and over again…with each diagnostic test we ran.
The month passed by slowly….I kept hitting a brick wall over and over again…with each diagnostic test we ran.
Vet2: This was Chance’s vet for many years and where Chance lived the summer I moved home. Vet1 was used because of connivence and due to being the vet of the owner of the farm. I called Vet2, desperate, and she came out to see him. Vet2 had always been amazing with Chance- kind, calm, and seems to act on intuition in conjunction with science. She ran a CBC, tested for Cushings, Lymes, an did x-rays on the back right leg.
RESULTS:
* Metabolic Syndrome- Cornell
GLUCOSE: 10mg/dl
LIPEMIA: 8mg/dl
HEMOLYSIS: 1mg/dl
ICTERUS: 2mg/dl
*Endocrinology
ACTH endo 21.4 pg/ml
INSULIN 15.22 uIU/ml
THYROXINE T4 baseline 0.77 ug/dl
*Lyme Mitpix- Cornel
OspA Value 1253- Equivocal
OspC Value 79- Negative
OspF Value 592- Negative
Temp: 99.1, HR: 42, RR: 12, No murmur
Received Potomac Rabies and Stanozanol 4ml 7 vit B12
The X-rays of his back right showed nothing that could cause his flare-ups. While his thyroid was a bit low, it was not clinically significant. He was negative for Lymes and Cushings. Next step, aside from pain management, is to call Vet3- the holistic approach.
