Spotting Lameness: The Game Plan
— Read on horsenetwork.com/2018/10/spotting-lameness-game-plan/
Category Archives: Hole in Tendon

Current Breakthroughs in Equine Research
Over the past 30 years the Grayson-Jockey Club Research Foundation has funneled nearly $20 million into studies aimed at improving horse health. This year the effort continues with funding for a dozen new projects in fields ranging from laminitis to lameness diagnosis. A sampling:
Detecting lameness at the gallop: Kevin Keegan, DVM, of the University of Missouri, is developing an objective method (using a calibrated instrument) for detecting obscure, subtle lameness in horses at the gallop. The goal is a low-cost method that can be used in the field to increase understanding of lameness in racehorses.
Deworming and vaccines: While it’s not unusual to deworm and vaccinate horses on the same day, recent findings have raised concerns about possible interactions. Martin Nielsen, DVM, of the University of Kentucky and Gluck Equine Research Center, is investigating whether deworming causes an inflammatory reaction that affects vaccination.
Imaging injured tendons: Horses recovering from tendon injuries are often put back to work too soon and suffer re-injury. Sabrina Brounts, DVM, of the University of Wisconsin–Madison, is exploring a new method developed at the university to monitor healing in the superficial digital flexor tendon. The technique, called acoustoelastography, relates ultrasound wave patterns to tissue stiffness: Healthy tendon tissue is stiffer than damaged tissue.
Detecting laminitis early: Hannah Galantino-Homer, VMD, of the University of Pennsylvania, is investigating possible serum biomarkers (molecular changes in blood) that appear in the earliest stages of laminitis. The goal is to develop tests for these disease markers so that treatment can start when laminitis is just developing, before it’s fullblown and damages the foot.
Other new studies include evaluations of a rapid test for salmonella; investigation of how neurologic and non-neurologic equine herpesvirus 1 (EHV-1) spreads cell-to-cell in the body; an effort to map the distribution of stem cells after direct injection into veins; and more.
This article originally appeared in the June 2013 issue of Practical Horseman.

Immune Booster Leads to Infection?
For the past 6 weeks, my horse has been receiving Ozonetherapy to aid in his chronic back leg related issues- dermatitis (“scratches”), previous DDFT tendon laceration, a history of Lymphingitis, and the residual scar tissue from his DDFT injury. Due to his age (27), he lacks proper circulation in his hind end which does not help him fight his pastern dermatitis.
According to the American Academy of Ozonetherapy, Ozonetherapy is described as;
“Ozonotherapy is the use of medical grade ozone, a highly reactive form of pure oxygen, to create a curative response in the body. The body has the potential to renew and regenerate itself. When it becomes sick it is because this potential has been blocked. The reactive properties of ozone stimulate the body to remove many of these impediments thus allowing the body to do what it does best – heal itself.”
“Ozonotherapy has been and continues to be used in European clinics and hospitals for over fifty years. It was even used here in the United States in a limited capacity in the early part of the 20th century. There are professional medical ozonotherapy societies in over ten countries worldwide. Recently, the International Scientific Committee on Ozonotherapy (ISCO3) was formed to help establish standardized scientific principles for ozonotherapy. The president of the AAO, Frank Shallenberger, MD is a founding member of the ISCO3.”
“Ozonotherapy was introduced into the United States in the early 80’s, and has been increasingly used in recent decades. It has been found useful in various diseases;
- It activates the immune system in infectious diseases.
- It improves the cellular utilization of oxygen that reduces ischemia in cardiovascular diseases, and in many of the infirmities of aging.
- It causes the release of growth factors that stimulate damaged joints and degenerative discs to regenerate.
- It can dramatically reduce or even eliminate many cases of chronic pain through its action on pain receptors.
- Published papers have demonstrated its healing effects on interstitial cystitis, chronic hepatitis, herpes infections, dental infections, diabetes, and macular degeneration.”
After doing research and speaking to one of my good friends, we determined that Chance’s flare up of Lymphingitis, after almost 3 years of not a single issue, could possibly be caused by his immune system’s response to Ozonetherapy. Let me explain.
Chance suffers from persistent Pastern dermatitis (“scratches”) since I purchased him in 2000. I have tried everything- antibiotics, every cream and ointment and spray for scratches, diaper rash ointment, iodine and vaseline mix, Swat, laser treatments, scrubs and shampoos, shaving the area, wrapping the area, light therapy…you name it, I have tried it. So, when we began Ozonetherapy to help break down the left over scar tissue from his old DDFT injury, I noticed that his scratches were drying up and falling off. We continued administering the Ozonetherapy once a week for about 6 weeks. The improvement was dramatic!
However, one day Chance woke up with severe swelling in his left hind leg and obviously, he had difficulty walking. He received Prevacox and was stall bound for 24 hours. The vet was called and she arranged to come out the following day. The next morning, Chance’s left leg was still huge and he was having trouble putting weight on it. I did the typical leg treatments- icing, wrapping. The swelling remained. I tried to get him out of his stall to cold hose his leg and give him a bath but he would not budge. He was sweaty and breathing heavily and intermittently shivering. So, I gave him an alcohol and water sponge bath and continued to ice his back legs. I sat with him for 4 hours waiting for the vet to arrive. He had a fever and wasn’t interested in eating and his gut sounds were not as audible. He was drinking, going to the bathroom, and engaging with me. I debated giving him Banamine but did not want it to mask anything when the vet did arrive.
The vet arrived, gave him a shot of Banamine and an antihistamine and confirmed that Chance had a fever of 102 degrees and had Lymphingitis. There was no visible abrasion, puncture, or lump… I asked the vet to do x-rays to ensure that he did not have a break in his leg. The x-rays confirmed that there was no break. The vet suggested a regiment of antibiotics, steroids (I really am against using steroids due to the short-term and long-term side effects but in this case, I would try anything to make sure he was comfortable) , prevacox, and a antacid to protect Chance from stomach related issues from the medications. It was also advised to continue to cold hose or ice and keep his legs wrapped and Chance stall bound.
The following day, Chance’s legs were still swollen but his fever had broken. The vet called to say that the CBC had come back and that his WBC was about 14,00o. She suggested that we stop the steroids and do the antibiotic 2x a day and add in Banamine. I asked her if she could order Baytril (a strong antibiotic that Chance has responded well to in the past) just in case. And that is what we did.
Being as Chance had such a strong reaction to whatever it was, I did some thinking, discussing, and researching…first and foremost, why did Chance have such an extreme flare up of Lymphingitis when he was the healthiest he has ever been? And especially since he had not had a flare up in 3+ years…plus, his scratches were getting better not worse. The Ozonetherapy boosted his immune system and should provide him with a stronger defense against bacteria, virus’, etc. So why exactly was he having a flare up? And that is when it hit me!
In the past when Chance began his regiment of Transfer Factor (an all natural immune booster), he broke out in hives. The vet had come out and she felt it was due to the Transfer Factor causing his immune system to become “too strong” and so it began fighting without there being anything to fight, thus the hives. My theory- Chance started the Ozonetherapy and his body began to fight off the scratches by boosting his immune system. As the treatments continued, his immune system began to attack the scratches tenfold. This resulted in his Lymphatic system to respond, his WBC to increase, and his body temperature to spike. Makes sense…but what can I do to ensure this is not going to happen again?
My friend suggested attacking the antibiotic resistant bacteria by out smarting them…okay, that seems simple enough…we researched the optimal enviroments for the 3 types of bacteria present where Chance’s scratches are (shown in the results of a past skin scape test). The bacteria – E. Coli, pseudomonas aeruginosa and providencia Rettgeri. The literature stated that PA was commonly found in individuals with diabetes…diabetes…SUGAR! How much sugar was in Chance’s feed? I looked and Nutrina Safe Choice Senior feed is low in sugar…so that is not it. What else can we find out? The optimal temperature for all three bacteria is around 37 degrees celsius (or 98.6 degrees fahrenheit), with a pH of 7.0, and a wet environment. Okay, so, a pH of 7.0 is a neutral. Which means if the external enviroment (the hind legs)pH is thrown off, either to an acidic or alkaline pH, the bacteria will not have the optimal enviroment to continue growing and multiplying. How can I change the pH?
Vinegar! An antimicrobial and a 5% acetic acid! And…vinegar is shown to help kill mycobacteria such as drug-resistant tuberculosis and an effective way to clean produce; it is considered the fastest, safest, and more effective than the use of antibacterial soap. Legend even says that in France during the Black Plague, four thieves were able to rob the homes of those sick with the plague and not become infected. They were said to have purchased a potion made of garlic soaked in vinegar which protected them. Variants of the recipe, now called “Four Thieves Vinegar” has continued to be passed down and used for hundreds of years (Hunter, R., 1894).
I went to the store, purchased distilled vinegar and a spray bottle and headed to the farm. I cleaned his scratches and sprayed the infected areas with vinegar. I am excited to see whether our hypothesis is correct or not…I will keep you posted!
References & Information
Effect of pH on Drug Resistent Bacteriaijs-43-1-174
What does my horse’s CBC mean?

Nutrena SC Senior feed ingredience
The American Academy of Ozonetherapy
Hunter, Robert (1894). The Encyclopaedic Dictionary. Toronto: T.J. Ford. ISBN 0-665-85186-3.

Fall Fever
Today Chance had swelling of his back right fetlock. He had a fever around 104 and didn’t eat his feed. His eyes were dull and he was lethargic. He wasn’t limping but was walking slower than normal (he usually runs to the paddock or back to the barn). I decided, due to the Lymphingitis flare up on his back right leg, I would give him a shot of 5 mls (or 5 cc) of Banamine and wrap his leg. Once the medication set in, I would bring him in to give him a bath (it was 80 degrees today). So, that is what I did. By the time he was back at the barn he was covered in sweat. I cold hosed him and drenched the wrap in cool water and let him roam around the barn.
Thankfully, the vet was able to meet me at her veterinary practice so that I could pick up Baytril and more Banamine. Since Chance just had Lyme Disease (and had finished his medication less than a week ago), we are not 100% if this is a Lyme reaction or something else. The plan is to administer 25 cc of Baytril either orally, in his feed, or via IV for 6 days and Banamine 10 mls (or a 1000 lbs) twice a day for 3 days. The vet suggested that I do 5 cc of Banamine if his fever remains between 101-103 degrees and 10 cc if his fever is 103 degrees or above. During this time I will begin Prevacox- one 1/4 of a tablet once a day. After 3 days, I will discontinue the Banamine and continue the Prevacox. If his fevers are not down in two days, I will continue the Baytril but start the doxycycline as it maybe a Lyme disease symptom.
While researching Lyme Disease, I found that many people do two+ months of doxycycline instead of 30 days to ensure the disease has been erraticated completely. However, since Chance had shown such improvement after 30 days, I decided to not do another month. Maybe I should have…
However, Chance had similar symptoms when we found a small laceration in the DDFT tendon of his back left hind- swelling, Lymphingitis, fever, lethargy, no appetite, etc. If he does have an issue with his tendon I will most likely do another round of Stem Cell treatments which proved to be helpful last time. Thankfully I stored his stem cells in a Stem Cell Bank (via Vet-Stem) and can easily have them shipped.
I have a limp!
Resources on how to diagnose, treat, prevent, and handle lameness in horses
Your Horse Has a Swollen Leg – Why and What To Do | EquiMed – Horse Health Matters
Fetlock Lameness – It’s importance… | The Horse Magazine – Australia’s Leading Equestrian Magazine
Causes of Equine Lameness | EquiMed – Horse Health Matters
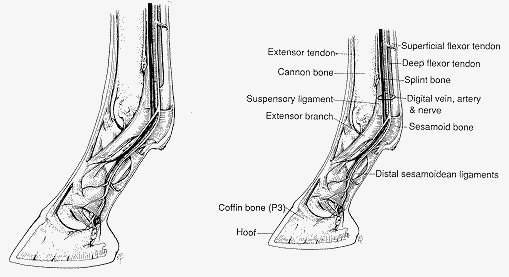
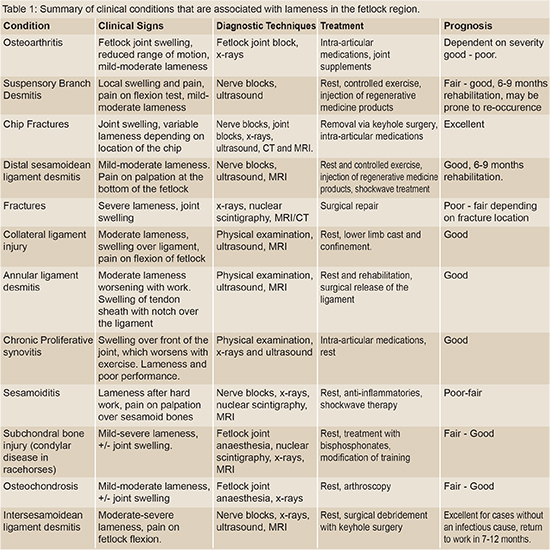
Common Causes of Lameness in the Fetlock

Equine Podiatry
Medical History
- DDFT Lesion on right hind
- Cervical Spine Arthritis
- Hip discomfort due to past fall
Past Treatments Tried
- Stem Cell Injections: Healed the DDFT lesion in right hind until recently the lesion began to reappear
- Ozone Therapy: Assists in the healing of tissues
- Shock Wave Therapy: Assists in the healing of tissue
- Chriopractic adjustments
- Acupuncture
- Supplements
Initial Consultation
Chance showed decreased movement in his right hip and a audible cracking noise at the suspensory joint. He has edema of both hind fetlocks, Pastern, and Pastern Dermatitis. Chance was unshawed on both hinds due to his inability to stand for long periods of time and his decreased mobility. However, his front adorned clips.
Due to the length of Chance’s front toes and the height of his heels he was unable to evenly distribute his weight (60/40) to his front and hind ends. This would most likely cause increased tension on the DDFT tendons and corresponding ligaments resulting in an increased likelihood of tendon and ligament related injuries. The uneven distribution of weight could also inhibit the horse’s range of motion through his hips resulting in his body compensating for this injury and causing ataxia (balance issues), pain, arthritic changes, and cervical spine misalignment.
By shortening the toe of both front feet, the heel will rise allowing a more even distribution of his weight.
Front


Final Product: Front
Trimmed feet to corrected to the following specifications:
Foot Beginning Angle & Toe Corrected Angles & Toe Total P.C.
L/F 47 Degrees at 3 7/8 inches 53 Degrees at 3 inches 6 Degrees
R/F 45 Degrees at 3 3/4 inches 54 Degrees at 3 inches 9 Degrees
Hind

Final Product: Hind

| Return visit to trim and shoe Chance’s hind feet with #2 OBRHB Wedge shoes.Trimmed hind feet and corrected to the following specifications:
Foot Beginning Angle & Toe Corrected Angles & Toe Total P.C. L/H 48 Degrees at 3 7/8 inches 54 Degrees at 3 1/4 inches 6 Degrees R/H 46 Degrees at 4 1/4 inches 55 Degrees at 3 1/4 inches 9 Degrees Note: Chance needed to be sedated by veterinarian to complete the trim and shoe his hind feet due to preexisting hip and DDFT issues. |

Ozone Therapy
OZONE THERAPY – HISTORY, PHYSIOLOGY, INDICATIONS, RESULTS
Judith M. Shoemaker, DVM 305 Nottingham Road Nottingham, PA 19362
717-529-0526 Fax 717-529-0776
http://www.judithshoemaker.com
Ozone therapy has been utilized and heavily studied for more than a century. Its effects are proven, consistent, safe and without side effects. Why is it not more universal in its use? Many of you have come with some trepidation about infusing a gas into a vessel because you are concerned about emboli, or have some dreadful fear about ozone’s toxicity since we frequently hear about the unhealthy ozone levels in the atmosphere. These fears do not apply to properly administered medical ozone, and the potential benefits of ozone therapy are profound and without associated detrimental effects.
Oxygen, in its several forms, cycles through the atmosphere and life processes just as water does. Ozone is produced in the upper atmosphere when UV light strikes the oxygen rising from plants, plankton, and algae in our forests and seas. It then falls back through the atmosphere, as it is heavier than air, combining with pollutants and water, cleaning the air and forming peroxides that benefit plants. Ultraviolet light breaking down pollutants and nitrous oxides also can produce ozone at the ground level, which is the eye and lung irritant in smog.
Medical ozone, used to disinfect and treat disease, has been around for over 150 years. Used to treat infections, wounds, and multiple diseases, ozone’s effectiveness has been well documented. Ozone has been used to disinfect drinking water since before the turn of the last century. A text on medical ozone therapy was published by Dr. Charles J. Kenworth in 1885! The best technology for producing ozone gas was designed and built by Nikola Tesla in the 1920’s. Heads of leading medical institutions in the U.S. contributed to a 1929 book “Ozone and Its Therapeutic Actions” describing the treatment of 114 diseases using ozone.
In 1933, the AMA began its systematic suppression of all modalities of treatment that did not complement its liaison with the emerging pharmacologic and diagnostic industries. Ozone therapy, along with many other useful therapies, were methodically eliminated from the educational process and exposure to the public in the U.S.
Less suppression has occurred in Europe and other countries, especially in Russia. Today in Germany, and other countries, ozone therapy is commonplace. Over 7000 doctors in Germany use it daily. In fact, in Germany, ozone generators are in ambulances for treatment of stroke victims. The incidence of permanent paralysis in these patients is much less than that in similar patients where ozone is not used.
Ozone generators are relatively simple and inexpensive. The equipment used to handle ozone is readily available but needs to be relatively non-reactive. Glass, Teflon, Kynar, silicon, and gold are completely non-reactive. Equipment made of other substances can contaminate the ozone or just deteriorate rapidly using up the ozone and becoming nonfunctional.
Generators use several technologies to produce ozone
- UV lamp – makes small amounts of ozone and is unreliable in making accurate concentrations. They burn out easily.
- Corona discharge – dual dielectric sealed systems produce ozone but also lots of heat which is both destructive to ozone and to the machine.
- Cold plasma generators – which produce ozone using low level current passed in 2 tubes of a noble gas between which an electrostatic plasma field forms that ionizes the oxygen.Ozone concentration is measured in u/ml or gms/L of oxygen, 5% or 70 u/ml is usually the maximum concentration used in clinical medical applications. High concentrations will damage red cells and inhibit growth of healthy cells.Dosage and frequency protocols vary widely. Initial high dose treatments may “jumpstart” the immune system followed by lower doses. Those who are fearful have been “starting slow and going low” with dosage and still have good results. Concentration must be carefully controlled with accurate flow rates, requiring pediatric regulators for the needed slow flow rates to produce high concentrations. Therefore, home made machines and lesser quality nonmedical devices are not appropriate.
Ozone poteniates free radical scavenging substances and systems in the body, inducing the production of superoxide dismutase, catalase, and glutathione peroxidase. If ozone administration causes any respiratory irritation from out-gassing through the lungs, a bolus dose of 1 to 5 grams of vitamin C can be given and will eliminate any coughing instantly.
Oxygen/ozone mixtures cannot cause emboli when injected at reasonable rates as they dissolve and diffuse very quickly in body fluids, unlike air (predominantly nitrogen) which is what forms emboli and causes the bends or decompression disease.
The physiologic actions of ozone are many, the simplest of which is to provide sufficient oxygen to allow complete oxidation of sugars and other fuels to produce sufficient and efficient energy and to “burn clean” to CO2, water, and inert end products. If not enough oxygen is available, then incomplete oxidation occurs, producing carbon monoxide, lactic acid, and partially oxidized toxins that inhibit further oxygen metabolism and “clog the system”, tying up hemoglobin, water, and the mechanisms for function and elimination.
Administration can be through any route with modifications:
- Direct IV infusion – Ozone slowly administered into a major vessel.
- Major auto-hemotherapy – Anticoagulated blood is mixed with ozone and is infused into a vessel.
- Rectal/vaginal insufflation – Humidified ozone is administered by catheter.
- Minor autohemotherapy – Blood mixed with ozone is injected intramuscularly.
- Limb or body bagging – Body or parts are bathed in humidified ozone.
- Ozonated water – Dissolves easily in water to be used topically or consumed.
- Ozone in Saline or LRS – Can be used topically or given IV or SQ.
- Intra-articular administration – For joint healing and prolotherapy.
- Prolo/Sclerotherapy – Very good, less painful than other agents.
- Acupuncture – With ozone, more effective than B12.
- Ozonated olive oil – Ozone is bubbled through oil until the oil is thickened. This will produce ozonides that are not irritating and thus is applied topically even to eyes.
- Inhalation – Ozone that has been bubbled through olive oil and humidified will not irritate respiratory epithelium.
- Subconjunctival injection – For ulcers and keratitis sicca.
- Gingival and tooth apex injection – Can eliminate infection.
- Urinary bladder insufflation – For chronic inflammation.
- Disc protrusions – Prolotherapy, which can be injected at interspinous space and around facets, stabilize joints and accelerate healing.
- Auricular – Can be direct, humidified, or bagged with a homemade device made from IV bags and tubing (á la Margo Roman).As an anticancer, antiviral, antibacterial, and ant fungal agent, ozone is unsurpassed, especially since there are no appreciable side effects.Oxygen deficit is key to the development and progression of all disease processes. Dr. Otto Warburg’s work, confirmed by others, shows that this deficit and subsequent toxin buildup is the fundamental cause of all degenerative disease, especially cancers.
Antioxidants help the body to protect itself from excessive oxidative damage caused by multiple free radicals, many of which are inactivated by ozone. The support of free radical scavenging systems is important but only oxygen can improve the deficit that makes cells vulnerable to oxidative damage in the first place. Long-term ozone therapy can be augmented by supplementation with antioxidants, but normally they should not be administered within 4 to 12 hours of ozone therapies.
Ozone produces the same effects as exercise, which produces significantly more free radical oxygen than can be administered in any ozone treatment. Ozone equals ”exercise in a syringe” without doing joint damage.
Ozone potentiates more complete oxidation, helps to maintain more normal body temperature and increases the effects of most hormones, vitamins, herbs, homeopathics, and drugs. Concurrent ozone administration reduces the amount of chemotherapeutic drugs needed to achieve effect by 1⁄4 to 3⁄4. It complements chelation therapies and frequently improves the affect and sense of well being in patients.
Continued therapy will allow Herring’s Law to manifest “Healing from inside to outside, top to bottom, front to rear, and in reverse chronological order of the insults to the body.” Healing crises, however, may occur. Ozone therapy facilitates the rapid resolution of these crises.
2005 Judith M. Shoemaker, DVM
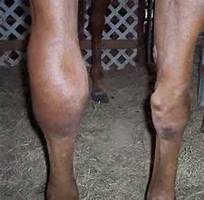
Treating Cellulitis in horses
A common and potentially hazardous infection that can be helped with combining antibiotics, cold hosing, and exercise.

On Monday night I showed up at the barn around 7:00 p.m. to ride once the day cooled off. To my dismay I found that Freedom’s knee was hugely swollen. I had wrapped his legs because he’d felt a bit stocked up the night before and because the swelling had no where to go except the knee, the effect was horrifying. Visualize a grapefruit.
Almost immediately I saw the cause: a scrape less than an inch long. Before I called the vet I scrubbed the wound to make sure it wasn’t a puncture wound (didn’t look like it to me, but a puncture would where a joint is involved can be very serious). Normally I would also shave the area around the cut but I had sent my clipper blades out to be sharpened! My guess was cellulitis but since it involved a joint I wanted to makes sure I…
View original post 499 more words

Pain in the Neck
My old guy has always had issues with his cervical spine/neck. Throughout the years he has developed arthritis which has caused symptoms which mirror EPM such as; ataxia, difficulty bending, hind end weakness, difficulty going up hills, lethargy, difficulty balancing when foot is lifted, muscle atrophy, sore back…you get the picture.
When his symptoms first came on I had the vet test for EPM. The test was positive. I did my research and found out that about 50% of horses will test positive for EPM but only 1% show actual impairment from the virus. I went ahead and completed two rounds of EPM medication therapy and still his symptoms continued. So, I sought out another vet who practiced eastern and western medicine.
After some chiropractic adjustments and acupuncture she felt that his issues were actually due to the cervical spine and not EPM. The vet also showed me how, when looking at Chance straight on, one of his eyes was lower then the other- a classic sign of cervical and jaw issues. We continued with the chiropractic and acupuncture therapy and have continued for over a year and the change has been remarkable. Along with these therapies, we upped his feed, added supplements, began stretches and different exercises, and had him walking and running up and down hills whenever he was outside. The dentist has also been of great help by floating Chance’s teeth every few months instead of once a year. This helps with the alignment of his teeth because he tends to ware one side of his teeth down more then the other; ultimately straining his jaw and neck.
He has rebuilt the muscle on his hind end, put on around 100 lbs, and is able to do stretches while someone is holding his foot up. He runs when he is outside and is no longer on pain medications (except on the rare occasion).
Here is some useful information on a horse’s back and cervical spine.
Diagnosing A Horse’s Neck Problems
Main Causes of Ataxia in Horses

Laser Time
A little over a year ago Chance was diagnosed and treated for a lesion on the Deep Digital Flexor Tendon (DDFT) of his hind fetlock. At the time, I decided to go with Stem Cell injections due to it being the least invasive treatment option. The Stem Cells worked wonders and Chance went from barely being able to walk to running up hills, from daily pain medications to a supplement (DuraLactin) to help with pain and inflammation) for arthritis.
A few months ago I wanted to see how Chance’s fetlock was holding up. He did not have any symptoms- no swelling, lameness, etc- but I wanted to make sure. The ultrasound revealed that he did still have a small lesion on his DDFT that the vet felt was “congenital” and not problematic. But due to his history I wanted to ensure that it stayed non-problematic. I invested in some protective and supportive hind boots for hi to wear when he is outside or stall bound due to weather and decided to do a round (about 5 sessions) of laser treatments on his hind leg. The laser treatments are relatively inexpensive (about $65.00), non-invasive, and pretty much risk free.
We are coming up on our 3rd treatment and due to Chance being asymptomatic it is hard to tell if they are beneficial until we do another ultrasound. Once an ultrasound is completed I will post more.
Article on Stem Cell Treatments: http://www.rossdales.com/news/new-stem-cell-trial-to-treat-deep-digital-flexor-tendon-injury.htm
Articles on Laser Treatments: Research Laser Therapy
When It Rains, It Pours
The other day I noticed that Chance’s back fetlock a were slightly swollen and he was visably stiffer then normal. I also noticed a golf ball sized lump in the middle of the his chest. It wasn’t super sensitive and looked like a tick bite reaction, except there was no tick and a tiny barely noticeable scratch.
I put a Poltace wrap on his back right leg (which was the leg he had previously injured and received stem cell injections in) and gave him some pain medication. I also started him on Baytril and Ulcerguard as a precaution as previously advised by the vet.
I made an appointment with our vet to come ultrasound his hind right leg and she was to come out in the next two days. I was incredibly anxious to say the least.
The vet arrived and explained that the lump on Chance’s chest was a hematoma from another horse biting him or from him hitting something. Nothing to worry about, it was just the pooling of fluids to lowest point.
I then trotted Chance back and forth as the vet watched. After an exam and the ultrasound, the vet explained that she felt that the swelling was due to Chance’s hip pain and the Pastern dermatitis that we have been treating and we’re finally coming off.
The ultrasound showed a tiny DDFT lesion (vet referred to as a defect that shouldn’t be causing any symptoms). The ultrasound also showed scar tissue that we need to get “stretched out” so that he can gain increased flexibility and work as a protection for Chance’s tendons and legiments. The ultrasound also showed some fluid build up as well. Chance’s Fetlock looks good as do his legiments.
The vet wants Chance to stay on Baytril and Ulcerguard until complete. She also has added a 5 day course of Benadryl and steroids to help with edema of back hind legs.
She also provided me with a shampoo that is milder to clean off scratches and apply swat after cleaning. The vet explained that she didn’t understand why people picked the scabs from the scratches because they’re super deep and pulling the scabs off does more harm than good.
The Vet commented on Chance’s weight gain and how great his skin looks gooded. She wants me to continue working on the scratches and continue doing physical therapy on hills to build up his hind end then get farrier out for back feet.
All and all I feel good about how Chance is doing and feeling. He is still full of energy, eats like he hasn’t eaten in a week, and his eyes and coat are bright. He is not on daily pain medication and is only given it when he is not feeling great. Aside from a few hiccups, Chance is loving life and being spoiled!
Trust Your Instincts
Chance being lunged after many years of not being lunged due to a DDFT injury and possible EPM treatments. He is still stiff and needs to build up the muscle in his hind end thus why he is being lunged. In addition to his chiropractic adjustments, acupuncture, stretches and massages, and all natural pain medication (MicroLactin), he is also doing physical therapy- walking over poles, walking serpentines, and walking up and down hills.
New Concerns Have Sprung
Chance is continuing to gain weight, although as I said in the previous post, he still needs to put on a good 50-75 lbs. As the days continue to get warmer, Chance’s arthritis seems to become more manageable for him; his stride is longer and he runs around (mostly after Lucky) more frequently.
Unfortunately, when the farrier came out about two weeks ago Chance was too stiff to get his back right shoe on. The farrier decided to come back out to try and re-shoe him and, during that time in between, Chance must have tweaked it…AGAIN!
While Chance did not have a shoe on his back right I kept it wrapped to provide some protection and also even out all of his hooves. However, when I arrived I noticed that Chance was significantly twisting his back right leg inward at the walk & it had some swelling. The swelling was not horrible but it was noticeable. I cold hosed his leg for about 45 minutes while I groomed him & gave him a dose of Equinox (pain medication) and Ulcer Guard. I put on his back leg wrap to help with reducing the swelling and provide some extra support. Chance did his neck stretches effortlessly and was baring weight on his back hind.
But as I was grooming him I noticed, on the left side his chest, he had patches of hair loss and dandruff. The area did not look red or inflamed, nor did it seem itchy or painful. So I continued grooming him and decided to put a call into the vet to come and check his leg and the hair loss.
Of course, I turned to Google to try and find out what exactly could be the cause of the patches of hair loss.
According to a handful of sources, there are a few possibilities for hair loss- mites or Lice, a vitamin deficiency, rain rot or crud, or even just his natural shedding tendency. A skin scrape would help to confirm what may be the cause.
As for the swelling of Chance’s back right leg, I decided to call our previous vet who collected and injected Chance’s DDFT with stem cells to heal the hole in his tendon. We have some stem cells left over and I wanted to see if injecting his leg again would be of any benefit. I also would like to get an ultrasound recheck to ensure that there is not another injury to his DDFT tendon sheath again.
The twisting of his back hind leg is worrisome as well.
Everything I have read about EPM states that horses can have a relapse in symptoms after treatment is complete. My concern is that the twisting are due to the neurological symptoms coming back since Chance’s EPM treatment has been finished for a little over two weeks….
Our current vet believes that Chance’s ataxia and twisting is not due to EPM but his cervical spine instead. Could the twisting be worse due to the swelling of his hind leg? Or is the swelling and the twisting two separate issues all together?

Progress
Chance BEFORE tendon injury diagnosis (I need to find the video where he was at his worse)
Chance AFTER Stem Cell Treatments
After 1 round of EPM Treatment
Chance AFTER 2 rounds of EPM Treatments (Need to get a better video) Before there was no way he would have been able to get up that hill.
Stem Cell Therapy
Cutting Edge Cell-Based Therapies for Horses
Regenerative therapies, such as stem-cell therapy and platelet-rich plasma, can help speed up healing in equine tendon and ligament injuries and make the repairs stronger.

Stem cells
Stem-cell therapy is one of several treatments that fall under the umbrella of regenerative medicine, a fast-growing field that’s creating major buzz in veterinary and human medical circles. These treatments use the body’s own repair tools with the goal of better healing. In this article you’ll find what you need to know about two regenerative treatments being used in horses, stem-cell therapy and platelet-rich plasma. For guidance we turned to Alison Stewart, DVM, an equine surgeon and stem-cell researcher at the University of Illinois, and Jamie Textor, DVM, an equine surgeon who is researching PRP at the University of California at Davis.
These treatments are exciting, but they are very much works in progress. Researchers are searching for the most effective ways to use them, and there are many questions about how?and how well?they work in different situations. They require specialized facilities and know-how that may not be available in every private veterinary practice. But they’re becoming more widely used, and if they live up to their promise, that trend will continue.
Stem-Cell Therapy
Stem cells are cells that have the potential to develop into some or many of the different specialized cells that make up body tissues, such as muscle, bone, blood and nerves. There are different kinds of these chameleonlike cells:
- Embryonic stem cells are derived from fertilized embryos. Taken early enough they are totipotent?they can develop into any tissue type, Dr. Stewart says. They go through several stages, becoming less able to differentiate as they mature.
- Induced pluripotent cells are adult cells that have been genetically reprogrammed in the lab so they behave like embryonic stem cells. Like embryonic stem cells, they proliferate readily and can differentiate into multiple tissue types. Researchers generated the first iPSCs less than five years ago and the first from horses only last year. They’re still exploring the potential of these cells.
- Adult stem cells are found in many organs and tissues, typically in small numbers. They are multipotent?not as versatile as embryonic stem cells but able to differentiate into at least three specific cell types. These cells seem to remain at rest for many years until called on to generate replacements for cells that are lost through normal wear and tear, injury or disease. They also produce a range of bioactive proteins, including growth factors and other agents that help repair damaged tissue.
The commercial stem-cell treatments available for horses ?today make use of adult mesenchymal stem cells, or MSCs, which can differentiate into bone, cartilage, fat and fibrous connective tissue. The cells are autologous?derived from the horse being treated. (Experimental treatments have also been done using donor, or allogenic, stem cells.)
“The commercial treatments are ?mainly being used for soft-tissue injuries??tendons and ligaments,” Dr. Stewart says. They are used less for joint problems generally, although some veterinarians think that they can be helpful for stifle injuries that involve a lot of soft-tissue damage.
Tendons and ligaments have different functions?tendons transfer the action of muscles to the skeleton, while ligaments lash bone to bone and keep joints from wobbling. But both are made up mostly of organized networks of dense, elastic connective tissue, rich in a tough protein called collagen. And they basically heal in the same way?that is, slowly and often poorly, with disorganized scar tissue in place of organized collagen fibers. This leaves your horse prone to reinjury.
MSC therapy may allow better repair, with more organized collagen and less scarring, Dr. Stewart says. Your horse will still need a lengthy layup and rehab period, though. The therapy seems to help most when it’s given in the first few weeks after an injury, during the time when healing is getting underway. It’s much less effective for longstanding or chronic conditions.
MSC Treatment. If you and your veterinarian decide to try stem-cell treatment for your horse’s injured tendon, the first step will be to collect MSCs. The cells are harvested from bone marrow or fat, depending on the treatment method used. This is done with your horse standing and sedated, with local anesthesia.
- For marrow-derived stem cells, a sample of bone marrow is aspirated (drawn with a special needle) from the horse’s sternum or hip. The marrow contains stem cells along with serum that’s rich in growth factors. It’s couriered to a laboratory where stem cells are extracted, cultured to expand the numbers, recombined with the serum and returned for injection. Usually 10 million cells are used to treat a tendon, Dr. Stewart says, and expansion can take two to three weeks. (VetCell, www.vetcell.com, a British company, developed the process and now offers it in North America through Equine Partners America, LLC, www.vetcellamericas.com.)
- For fat-derived stem cells, the veterinarian makes an incision, usually near your horse’s tailhead, and collects a sample of fat tissue. The sample goes to a lab where it’s treated with enzymes and spun in a centrifuge to separate nucleated cells from the fat that makes up most of the tissue. The nucleated cell fraction (which may include MSCs and some adult fat cells) can be sent back for use within three days or kept and cultured to get a higher concentration of MSCs. (Vet-Stem, www.vet-stem.com, in Poway, California, is a leading provider of this service in the United States.)
Does it matter where stem cells are collected and how they’re processed? “Some would say yes, but there has been no head-to-head comparison of the long-term effects,” Dr. Stewart says. The various stem-cell products are handled in much the same way when they come back from the lab:

After stem cells are havested and processed, they are injected directly into the injury site.
In most cases the veterinarian injects the stem-cell product directly into the injured tissue, using ultrasound to guide the injection into the lesion. The treatment also can be delivered into the blood supply around the site (regional limb perfusion), but this may not be as effective. “A study comparing the two methods found many more MSCs at the lesion when they were injected directly at the site than when ?injected using regional limb perfusion,” says Dr. Stewart.
The cost varies. “In most cases, from harvesting to reinjection, you’re looking at $1,200 to $2,000 to treat a tendon ?injury,” Dr. Stewart says.
Side effects are rare. As with any injection, there’s a small risk of transient inflammation or infection. But with autologous cells there should be no immunogenic reaction?that is, your horse’s immune system won’t target the cells as foreign and try to destroy them. “Even with cells from another horse, MSCs should be less immunogenic than adult cells,” Dr Stewart says. “But studies are still being done on this.”
Will It Help? Stem-cell success stories abound, but there’s not much peer-reviewed scientific research comparing outcomes with stem cells and traditional treatments. Researchers have done postmortem tissue studies that show good results in tendon and ligament injuries, ?including better alignment of fibers and less disorganized scar tissue?but benefits are hard to track in living horses because of individual differences in their injuries and care, Dr. Stewart says.

Four ultrasound sacans of an injured superficial digital tendon. You can see a large lesion in the scan at the time the bone-marrow aspiration takes place. There is some degradation a month later when the stem cells are implanted and then clear improvement two and four months post-implantation as the tendon regenerates.A recent follow-up study showed lower rates of injury after MSC treatment. Dr. Roger Smith, a professor of equine ?orthopedics at the Royal Veterinary College in Britain and developer of the VetCell technique, reviewed outcomes in 113 racing Thoroughbreds with core lesions in the superficial digital flexor tendons and found that treatment with marrow-derived MSCs cut reinjury rates by more than half. Horses who returned to training after stem-cell treatment and were followed up for three years had a reinjury rate of 27 percent, compared to 57 percent in conventionally treated horses. No comparable follow-up study has been done with fat-derived cells, Dr. Stewart says.
Stem cell therapy is evolving, and researchers are still trying to determine exactly what the cells do after they’re ?injected. “Early research evaluated MSCs for their potential to replace damaged tissue,” Dr. Stewart says. “More research now is directed at their ability to modulate inflammation and encourage healing.”
How long they hang around the injection site varies with the cell type and the tissue. “In tendon, bone-marrow-derived MSCs seem to be present up to two weeks, and then the numbers drop off. We don’t know if they’ve migrated somewhere else, died or divided so that the dye marking them no longer shows up,” Dr. Stewart says. “Embryoniclike stem cells seem to persist longer at the site of injection and travel farther, but they’re not yet commercially available.”
The cells don’t always behave as ?expected. Veterinarians at Cornell University tracked bone-marrow-derived MSCs injected into the fetlock or stifle joints of healthy and arthritic horses. They hoped the stem cells would migrate into damaged cartilage, where they might help repair it. Instead, the cells went to the synovial membrane, which surrounds the joint.
Platelet-Rich Plasma

Platelet-rich plasma is blood plasma that has been enriched with platelets. PRP contains and releases several types of growth factors that stimulate soft-tissue healing.PRP is plasma (the straw-colored liquid portion of blood) with a high concentration of platelets, small cell fragments that circulate in the blood. Platelets are best known for their role in helping blood clot, but they also release high concentrations of growth factors that encourage healing. Injected into injured tissue, the premise is, PRP delivers a potent cocktail of these healing proteins to help stimulate tissue repair. This treatment has been used in dentistry for jaw repair and in human sports medicine. In horses, it’s being used primarily for tendon and ligament injuries, both alone and along with MSC therapy.
“We think acute lesions are most likely to benefit from PRP,” says Dr. Textor. “Chronic, degenerative tendon conditions are less likely to respond.” The ideal time for treatment isn’t known, she adds, “but three to four weeks after an injury is probably a good target.”
PRP has been tried as a way to spur wound healing in horses, but it doesn’t appear to help and may actually increase proud flesh formation, Dr. Textor says. It has also been tried as an equine joint treatment; but another blood-derived treatment, IRAP, is more often used there. (IRAP stands for interleukin-1 receptor antagonist protein, a substance that blocks a specific inflammatory agent involved in the erosion of cartilage.)
PRP Treatment. If you opt for this treatment, the PRP will be prepared in the clinic from your horse’s own blood.
A sample of blood is drawn and spun in a centrifuge to separate the plasma and platelets from the red blood cells and most of the white blood cells. The plasma is then concentrated so it contains higher-than-normal blood levels of platelets.
It’s ready for injection into the injury the same day, often in less than an hour.
The cost of a single treatment typically ranges from $400 to $1,000, depending on the veterinarian’s preparation method, Dr. Textor says.
As with stem-cell therapy and any other injection, there’s a small risk of infection or a brief flare of inflammation?but because PRP is derived from your horse’s own blood, the risks of an immunogenic reaction to the treatment are low.
Will It Help? PRP has several advantages?it’s easy to collect and prepare, the turnaround time (from harvest to reinjection) is short and the treatment is cheaper than stem-cell therapy. Those plusses are helping PRP gain acceptance in the horse world.
As with stem cells, though, there’s little published research on effectiveness. In a study of horses with experimentally created tendon lesions, Dutch researchers showed that a single PRP injection resulted in improved healing and increased tendon strength at six months. In a clinical study of racing Standardbreds with severe suspensory ligament lesions, Ohio State University researchers found that one PRP injection helped horses recover and return to racing. On the other hand, some studies in human medicine have cast doubt on PRP’s effectiveness in shoulder and Achilles tendon injuries.
The reasons for different outcomes may emerge with answers to some of the many questions about how the treatment works and how it should be given. For example:
- Do tendon injuries benefit from more than one injection? “We don’t know,” Dr. Textor says. “Many vets are using multiple injections.”
- Do injected platelets stay at the injury site after injection, pumping out growth factors as they do when activated naturally? They might be quickly cleared from the site by macrophages, the cells that “eat” other dying cells or tissue debris, Dr. Textor says. “We are looking into this question now to find out whether the physical presence of platelets is required at the site or whether we can just administer the growth factors derived from them.”
- How do different preparation and treatment methods affect outcomes? “There is so much variety in methods of PRP use, both in humans and in horses, that the results are becoming more and more difficult to interpret,” Dr. Textor says. For example, the platelets must be activated to release growth factors. That can be done in different ways?by exposing them to the clotting protein thrombin or to calcium, or by freezing and thawing, for example.
“The main focus of my research is in trying to identify all the variables that go into PRP preparation and administration and figuring out what is the best way to do things so we can standardize our methods and be consistent as practitioners,” Textor says. “It may be that better results are achievable once we figure out how to maximize the benefit of PRP.”
Looking Ahead
Here’s one thing that seems certain: There will be new developments in this rapidly growing field.
- “Researchers will continue to work on treatments for soft-tissue damage,” Dr. Stewart says. They’ll explore different preparation and delivery techniques and look for ways to prove the action and ?retention of stem cells in injured tissue.
- Cell-based therapies also hold promise for use against osteoarthritis, in which the cartilage lining the joint surfaces breaks down. So far stem-cell therapy has been less ?effective than hoped for this problem, Dr. Stewart says. Researchers are still investigating how to coax the cells to stimulate cartilage repair. One technique being ?explored combines them with PRP. Research is also being done on the use of stem cells for fracture repair, but practical treatments aren’t yet available for that.
- Also on the horizon?or maybe a bit beyond it?are potential regenerative treatments for other diseases, including laminitis. “Studies haven’t been done yet, but there are some reports of successful laminitis treatment with high doses of MSCs. There’s interest, so it’s likely that research will be done,” Dr. Stewart says. “There is also interest in looking at MSC use in neurologic conditions.”
- New sources of stem cells may come into use. For example, MSCs can be ?obtained from the umbilical cord ?moments after a foal is born. These cells are not yet used commercially, but forward-thinking horse owners can bank foal cord blood and tissue at the UC Davis Regenerative Medicine Laboratory.
Interest in human regenerative medicine is helping to fuel (and fund) a lot of the research into cell-based treatments for horses. People, like horses, heal slowly and often poorly after damage to tendons, ligaments, cartilage and bone?so the horse is an excellent research model for these treatments. That means research underway now may one day benefit you as well as your horse.
Learn more about tendon and ligament injuries.
Reprinted from the February 2012 issue of Practical Horseman magazine.
– See more at: http://practicalhorsemanmag.com/article/cutting-edge-cell-based-therapies-for-horses#sthash.UPnO5o1D.dpuf



