Spotting Lameness: The Game Plan
— Read on horsenetwork.com/2018/10/spotting-lameness-game-plan/
Tag Archives: Stem cell
New Concerns Have Sprung
Chance is continuing to gain weight, although as I said in the previous post, he still needs to put on a good 50-75 lbs. As the days continue to get warmer, Chance’s arthritis seems to become more manageable for him; his stride is longer and he runs around (mostly after Lucky) more frequently.
Unfortunately, when the farrier came out about two weeks ago Chance was too stiff to get his back right shoe on. The farrier decided to come back out to try and re-shoe him and, during that time in between, Chance must have tweaked it…AGAIN!
While Chance did not have a shoe on his back right I kept it wrapped to provide some protection and also even out all of his hooves. However, when I arrived I noticed that Chance was significantly twisting his back right leg inward at the walk & it had some swelling. The swelling was not horrible but it was noticeable. I cold hosed his leg for about 45 minutes while I groomed him & gave him a dose of Equinox (pain medication) and Ulcer Guard. I put on his back leg wrap to help with reducing the swelling and provide some extra support. Chance did his neck stretches effortlessly and was baring weight on his back hind.
But as I was grooming him I noticed, on the left side his chest, he had patches of hair loss and dandruff. The area did not look red or inflamed, nor did it seem itchy or painful. So I continued grooming him and decided to put a call into the vet to come and check his leg and the hair loss.
Of course, I turned to Google to try and find out what exactly could be the cause of the patches of hair loss.
According to a handful of sources, there are a few possibilities for hair loss- mites or Lice, a vitamin deficiency, rain rot or crud, or even just his natural shedding tendency. A skin scrape would help to confirm what may be the cause.
As for the swelling of Chance’s back right leg, I decided to call our previous vet who collected and injected Chance’s DDFT with stem cells to heal the hole in his tendon. We have some stem cells left over and I wanted to see if injecting his leg again would be of any benefit. I also would like to get an ultrasound recheck to ensure that there is not another injury to his DDFT tendon sheath again.
The twisting of his back hind leg is worrisome as well.
Everything I have read about EPM states that horses can have a relapse in symptoms after treatment is complete. My concern is that the twisting are due to the neurological symptoms coming back since Chance’s EPM treatment has been finished for a little over two weeks….
Our current vet believes that Chance’s ataxia and twisting is not due to EPM but his cervical spine instead. Could the twisting be worse due to the swelling of his hind leg? Or is the swelling and the twisting two separate issues all together?
Wide Open Spaces
What a difference almost a year can make!
Stem Cell Therapy
Cutting Edge Cell-Based Therapies for Horses
Regenerative therapies, such as stem-cell therapy and platelet-rich plasma, can help speed up healing in equine tendon and ligament injuries and make the repairs stronger.

Stem cells
Stem-cell therapy is one of several treatments that fall under the umbrella of regenerative medicine, a fast-growing field that’s creating major buzz in veterinary and human medical circles. These treatments use the body’s own repair tools with the goal of better healing. In this article you’ll find what you need to know about two regenerative treatments being used in horses, stem-cell therapy and platelet-rich plasma. For guidance we turned to Alison Stewart, DVM, an equine surgeon and stem-cell researcher at the University of Illinois, and Jamie Textor, DVM, an equine surgeon who is researching PRP at the University of California at Davis.
These treatments are exciting, but they are very much works in progress. Researchers are searching for the most effective ways to use them, and there are many questions about how?and how well?they work in different situations. They require specialized facilities and know-how that may not be available in every private veterinary practice. But they’re becoming more widely used, and if they live up to their promise, that trend will continue.
Stem-Cell Therapy
Stem cells are cells that have the potential to develop into some or many of the different specialized cells that make up body tissues, such as muscle, bone, blood and nerves. There are different kinds of these chameleonlike cells:
- Embryonic stem cells are derived from fertilized embryos. Taken early enough they are totipotent?they can develop into any tissue type, Dr. Stewart says. They go through several stages, becoming less able to differentiate as they mature.
- Induced pluripotent cells are adult cells that have been genetically reprogrammed in the lab so they behave like embryonic stem cells. Like embryonic stem cells, they proliferate readily and can differentiate into multiple tissue types. Researchers generated the first iPSCs less than five years ago and the first from horses only last year. They’re still exploring the potential of these cells.
- Adult stem cells are found in many organs and tissues, typically in small numbers. They are multipotent?not as versatile as embryonic stem cells but able to differentiate into at least three specific cell types. These cells seem to remain at rest for many years until called on to generate replacements for cells that are lost through normal wear and tear, injury or disease. They also produce a range of bioactive proteins, including growth factors and other agents that help repair damaged tissue.
The commercial stem-cell treatments available for horses ?today make use of adult mesenchymal stem cells, or MSCs, which can differentiate into bone, cartilage, fat and fibrous connective tissue. The cells are autologous?derived from the horse being treated. (Experimental treatments have also been done using donor, or allogenic, stem cells.)
“The commercial treatments are ?mainly being used for soft-tissue injuries??tendons and ligaments,” Dr. Stewart says. They are used less for joint problems generally, although some veterinarians think that they can be helpful for stifle injuries that involve a lot of soft-tissue damage.
Tendons and ligaments have different functions?tendons transfer the action of muscles to the skeleton, while ligaments lash bone to bone and keep joints from wobbling. But both are made up mostly of organized networks of dense, elastic connective tissue, rich in a tough protein called collagen. And they basically heal in the same way?that is, slowly and often poorly, with disorganized scar tissue in place of organized collagen fibers. This leaves your horse prone to reinjury.
MSC therapy may allow better repair, with more organized collagen and less scarring, Dr. Stewart says. Your horse will still need a lengthy layup and rehab period, though. The therapy seems to help most when it’s given in the first few weeks after an injury, during the time when healing is getting underway. It’s much less effective for longstanding or chronic conditions.
MSC Treatment. If you and your veterinarian decide to try stem-cell treatment for your horse’s injured tendon, the first step will be to collect MSCs. The cells are harvested from bone marrow or fat, depending on the treatment method used. This is done with your horse standing and sedated, with local anesthesia.
- For marrow-derived stem cells, a sample of bone marrow is aspirated (drawn with a special needle) from the horse’s sternum or hip. The marrow contains stem cells along with serum that’s rich in growth factors. It’s couriered to a laboratory where stem cells are extracted, cultured to expand the numbers, recombined with the serum and returned for injection. Usually 10 million cells are used to treat a tendon, Dr. Stewart says, and expansion can take two to three weeks. (VetCell, www.vetcell.com, a British company, developed the process and now offers it in North America through Equine Partners America, LLC, www.vetcellamericas.com.)
- For fat-derived stem cells, the veterinarian makes an incision, usually near your horse’s tailhead, and collects a sample of fat tissue. The sample goes to a lab where it’s treated with enzymes and spun in a centrifuge to separate nucleated cells from the fat that makes up most of the tissue. The nucleated cell fraction (which may include MSCs and some adult fat cells) can be sent back for use within three days or kept and cultured to get a higher concentration of MSCs. (Vet-Stem, www.vet-stem.com, in Poway, California, is a leading provider of this service in the United States.)
Does it matter where stem cells are collected and how they’re processed? “Some would say yes, but there has been no head-to-head comparison of the long-term effects,” Dr. Stewart says. The various stem-cell products are handled in much the same way when they come back from the lab:

After stem cells are havested and processed, they are injected directly into the injury site.
In most cases the veterinarian injects the stem-cell product directly into the injured tissue, using ultrasound to guide the injection into the lesion. The treatment also can be delivered into the blood supply around the site (regional limb perfusion), but this may not be as effective. “A study comparing the two methods found many more MSCs at the lesion when they were injected directly at the site than when ?injected using regional limb perfusion,” says Dr. Stewart.
The cost varies. “In most cases, from harvesting to reinjection, you’re looking at $1,200 to $2,000 to treat a tendon ?injury,” Dr. Stewart says.
Side effects are rare. As with any injection, there’s a small risk of transient inflammation or infection. But with autologous cells there should be no immunogenic reaction?that is, your horse’s immune system won’t target the cells as foreign and try to destroy them. “Even with cells from another horse, MSCs should be less immunogenic than adult cells,” Dr Stewart says. “But studies are still being done on this.”
Will It Help? Stem-cell success stories abound, but there’s not much peer-reviewed scientific research comparing outcomes with stem cells and traditional treatments. Researchers have done postmortem tissue studies that show good results in tendon and ligament injuries, ?including better alignment of fibers and less disorganized scar tissue?but benefits are hard to track in living horses because of individual differences in their injuries and care, Dr. Stewart says.

Four ultrasound sacans of an injured superficial digital tendon. You can see a large lesion in the scan at the time the bone-marrow aspiration takes place. There is some degradation a month later when the stem cells are implanted and then clear improvement two and four months post-implantation as the tendon regenerates.A recent follow-up study showed lower rates of injury after MSC treatment. Dr. Roger Smith, a professor of equine ?orthopedics at the Royal Veterinary College in Britain and developer of the VetCell technique, reviewed outcomes in 113 racing Thoroughbreds with core lesions in the superficial digital flexor tendons and found that treatment with marrow-derived MSCs cut reinjury rates by more than half. Horses who returned to training after stem-cell treatment and were followed up for three years had a reinjury rate of 27 percent, compared to 57 percent in conventionally treated horses. No comparable follow-up study has been done with fat-derived cells, Dr. Stewart says.
Stem cell therapy is evolving, and researchers are still trying to determine exactly what the cells do after they’re ?injected. “Early research evaluated MSCs for their potential to replace damaged tissue,” Dr. Stewart says. “More research now is directed at their ability to modulate inflammation and encourage healing.”
How long they hang around the injection site varies with the cell type and the tissue. “In tendon, bone-marrow-derived MSCs seem to be present up to two weeks, and then the numbers drop off. We don’t know if they’ve migrated somewhere else, died or divided so that the dye marking them no longer shows up,” Dr. Stewart says. “Embryoniclike stem cells seem to persist longer at the site of injection and travel farther, but they’re not yet commercially available.”
The cells don’t always behave as ?expected. Veterinarians at Cornell University tracked bone-marrow-derived MSCs injected into the fetlock or stifle joints of healthy and arthritic horses. They hoped the stem cells would migrate into damaged cartilage, where they might help repair it. Instead, the cells went to the synovial membrane, which surrounds the joint.
Platelet-Rich Plasma

Platelet-rich plasma is blood plasma that has been enriched with platelets. PRP contains and releases several types of growth factors that stimulate soft-tissue healing.PRP is plasma (the straw-colored liquid portion of blood) with a high concentration of platelets, small cell fragments that circulate in the blood. Platelets are best known for their role in helping blood clot, but they also release high concentrations of growth factors that encourage healing. Injected into injured tissue, the premise is, PRP delivers a potent cocktail of these healing proteins to help stimulate tissue repair. This treatment has been used in dentistry for jaw repair and in human sports medicine. In horses, it’s being used primarily for tendon and ligament injuries, both alone and along with MSC therapy.
“We think acute lesions are most likely to benefit from PRP,” says Dr. Textor. “Chronic, degenerative tendon conditions are less likely to respond.” The ideal time for treatment isn’t known, she adds, “but three to four weeks after an injury is probably a good target.”
PRP has been tried as a way to spur wound healing in horses, but it doesn’t appear to help and may actually increase proud flesh formation, Dr. Textor says. It has also been tried as an equine joint treatment; but another blood-derived treatment, IRAP, is more often used there. (IRAP stands for interleukin-1 receptor antagonist protein, a substance that blocks a specific inflammatory agent involved in the erosion of cartilage.)
PRP Treatment. If you opt for this treatment, the PRP will be prepared in the clinic from your horse’s own blood.
A sample of blood is drawn and spun in a centrifuge to separate the plasma and platelets from the red blood cells and most of the white blood cells. The plasma is then concentrated so it contains higher-than-normal blood levels of platelets.
It’s ready for injection into the injury the same day, often in less than an hour.
The cost of a single treatment typically ranges from $400 to $1,000, depending on the veterinarian’s preparation method, Dr. Textor says.
As with stem-cell therapy and any other injection, there’s a small risk of infection or a brief flare of inflammation?but because PRP is derived from your horse’s own blood, the risks of an immunogenic reaction to the treatment are low.
Will It Help? PRP has several advantages?it’s easy to collect and prepare, the turnaround time (from harvest to reinjection) is short and the treatment is cheaper than stem-cell therapy. Those plusses are helping PRP gain acceptance in the horse world.
As with stem cells, though, there’s little published research on effectiveness. In a study of horses with experimentally created tendon lesions, Dutch researchers showed that a single PRP injection resulted in improved healing and increased tendon strength at six months. In a clinical study of racing Standardbreds with severe suspensory ligament lesions, Ohio State University researchers found that one PRP injection helped horses recover and return to racing. On the other hand, some studies in human medicine have cast doubt on PRP’s effectiveness in shoulder and Achilles tendon injuries.
The reasons for different outcomes may emerge with answers to some of the many questions about how the treatment works and how it should be given. For example:
- Do tendon injuries benefit from more than one injection? “We don’t know,” Dr. Textor says. “Many vets are using multiple injections.”
- Do injected platelets stay at the injury site after injection, pumping out growth factors as they do when activated naturally? They might be quickly cleared from the site by macrophages, the cells that “eat” other dying cells or tissue debris, Dr. Textor says. “We are looking into this question now to find out whether the physical presence of platelets is required at the site or whether we can just administer the growth factors derived from them.”
- How do different preparation and treatment methods affect outcomes? “There is so much variety in methods of PRP use, both in humans and in horses, that the results are becoming more and more difficult to interpret,” Dr. Textor says. For example, the platelets must be activated to release growth factors. That can be done in different ways?by exposing them to the clotting protein thrombin or to calcium, or by freezing and thawing, for example.
“The main focus of my research is in trying to identify all the variables that go into PRP preparation and administration and figuring out what is the best way to do things so we can standardize our methods and be consistent as practitioners,” Textor says. “It may be that better results are achievable once we figure out how to maximize the benefit of PRP.”
Looking Ahead
Here’s one thing that seems certain: There will be new developments in this rapidly growing field.
- “Researchers will continue to work on treatments for soft-tissue damage,” Dr. Stewart says. They’ll explore different preparation and delivery techniques and look for ways to prove the action and ?retention of stem cells in injured tissue.
- Cell-based therapies also hold promise for use against osteoarthritis, in which the cartilage lining the joint surfaces breaks down. So far stem-cell therapy has been less ?effective than hoped for this problem, Dr. Stewart says. Researchers are still investigating how to coax the cells to stimulate cartilage repair. One technique being ?explored combines them with PRP. Research is also being done on the use of stem cells for fracture repair, but practical treatments aren’t yet available for that.
- Also on the horizon?or maybe a bit beyond it?are potential regenerative treatments for other diseases, including laminitis. “Studies haven’t been done yet, but there are some reports of successful laminitis treatment with high doses of MSCs. There’s interest, so it’s likely that research will be done,” Dr. Stewart says. “There is also interest in looking at MSC use in neurologic conditions.”
- New sources of stem cells may come into use. For example, MSCs can be ?obtained from the umbilical cord ?moments after a foal is born. These cells are not yet used commercially, but forward-thinking horse owners can bank foal cord blood and tissue at the UC Davis Regenerative Medicine Laboratory.
Interest in human regenerative medicine is helping to fuel (and fund) a lot of the research into cell-based treatments for horses. People, like horses, heal slowly and often poorly after damage to tendons, ligaments, cartilage and bone?so the horse is an excellent research model for these treatments. That means research underway now may one day benefit you as well as your horse.
Learn more about tendon and ligament injuries.
Reprinted from the February 2012 issue of Practical Horseman magazine.
– See more at: http://practicalhorsemanmag.com/article/cutting-edge-cell-based-therapies-for-horses#sthash.UPnO5o1D.dpuf
Stem Cell Injections
We decided to go ahead with the Stem Cell injections through the company Vet-Stem. Though expensive, they carry virtually zero risk, aside from a site infection, in comparison to the surgery.
Vet4 will gather the cells from his rear and stitch up the incisions made. From there, if there are enough cells, the culture will be sent to the lab, and in about two days, they are able to be injected into the leg!
UPDATE:
There were enough Stem Cells to inject! Chance is doing extremely well and is able to come home in a few days!!!
I asked if Vet4 could get Chance supportive back shoes before he left and he said he would.
Time to set up a trailer and get his stall ready in Sperryville!!!!
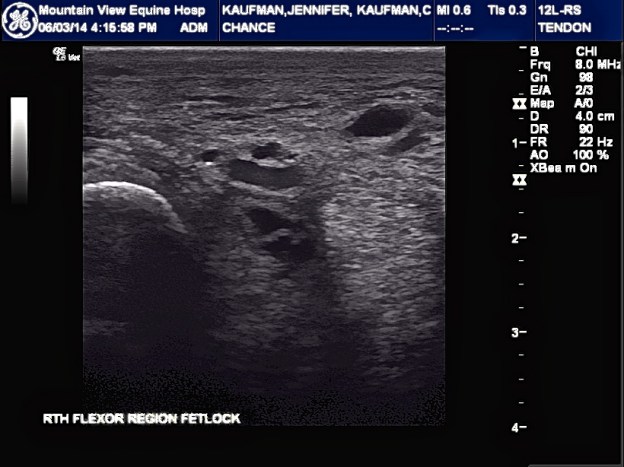
DDFT Lesions
Text from Vet4 after ultra sound #3:
“I can see that he has a deep digital flexor tendon lesion and the medial side of the tendon sheath has improve but lateral side is about the same. The DDFT may the cause of all this in the first place and everything else is secondary. We will re ultrasound in 10 days or so just to confirm my findings. If they are correct, it would help to treat that area.”
Conversation with Vet4 :
So far, Chance has received; shock wave therapy, compression therapy and laser therapy.
Chance has a hole in his tendon. Vet4 believes that this is due to an infection/bowed tendon and severe lameness. The ultrasound, done yesterday, shows no change in size of the tendon hole after the previous two rounds of injections.
“Lymphangitis is a symptom rather than a cause and the cause was never treated.” Vet1 continued to treat it like a disorder rather than a symptom!
The swelling and infection have dissipated, as has the severity of the lameness. Though still lame, he is running around in the pasture.
Pain meds were started again due to increased discomfort and soreness.
Vet4 suggests doing one of the following:
1. Stem cell- which can take about two days if sample drawn has enough stem cells. If not, it could take about 4-6 wks to culture. Once injected he can move home. He is to be hand walked for a few days and then can go out as normal. Vet4 will come out in about a month to do another ultrasound and, depending on the size of the hole, may need to do further injections.
2. Surgery to clean out but NOT repair the tendon. This was not discussed in detail.
Payment plans may be an option. I emailed the office for payment options.
Time to make another decision!

Coming Home to Love & Peace
Chance was able to come home a week later. Sam & John went to pick him up at the hospital. However, upon arriving, they soon found out that Chance did not want to get on the trailer. Sam later told me that one of my sweatshirts was in the truck, so she brought it out and let him smell it- he finally loaded.
I got his stall ready- tons of fresh shavings, hay, a new water bucket…
The moment he got off of the trailer he was shaking! I gave him a warm bath and let him out in a small, flat paddock so he could be in the sunshine.
This is what happened when I let him out! He did something he had not been capable of doing for months and months, if not longer.



