
Category Archives: Mud Fever


Immune Booster Leads to Infection?
For the past 6 weeks, my horse has been receiving Ozonetherapy to aid in his chronic back leg related issues- dermatitis (“scratches”), previous DDFT tendon laceration, a history of Lymphingitis, and the residual scar tissue from his DDFT injury. Due to his age (27), he lacks proper circulation in his hind end which does not help him fight his pastern dermatitis.
According to the American Academy of Ozonetherapy, Ozonetherapy is described as;
“Ozonotherapy is the use of medical grade ozone, a highly reactive form of pure oxygen, to create a curative response in the body. The body has the potential to renew and regenerate itself. When it becomes sick it is because this potential has been blocked. The reactive properties of ozone stimulate the body to remove many of these impediments thus allowing the body to do what it does best – heal itself.”
“Ozonotherapy has been and continues to be used in European clinics and hospitals for over fifty years. It was even used here in the United States in a limited capacity in the early part of the 20th century. There are professional medical ozonotherapy societies in over ten countries worldwide. Recently, the International Scientific Committee on Ozonotherapy (ISCO3) was formed to help establish standardized scientific principles for ozonotherapy. The president of the AAO, Frank Shallenberger, MD is a founding member of the ISCO3.”
“Ozonotherapy was introduced into the United States in the early 80’s, and has been increasingly used in recent decades. It has been found useful in various diseases;
- It activates the immune system in infectious diseases.
- It improves the cellular utilization of oxygen that reduces ischemia in cardiovascular diseases, and in many of the infirmities of aging.
- It causes the release of growth factors that stimulate damaged joints and degenerative discs to regenerate.
- It can dramatically reduce or even eliminate many cases of chronic pain through its action on pain receptors.
- Published papers have demonstrated its healing effects on interstitial cystitis, chronic hepatitis, herpes infections, dental infections, diabetes, and macular degeneration.”
After doing research and speaking to one of my good friends, we determined that Chance’s flare up of Lymphingitis, after almost 3 years of not a single issue, could possibly be caused by his immune system’s response to Ozonetherapy. Let me explain.
Chance suffers from persistent Pastern dermatitis (“scratches”) since I purchased him in 2000. I have tried everything- antibiotics, every cream and ointment and spray for scratches, diaper rash ointment, iodine and vaseline mix, Swat, laser treatments, scrubs and shampoos, shaving the area, wrapping the area, light therapy…you name it, I have tried it. So, when we began Ozonetherapy to help break down the left over scar tissue from his old DDFT injury, I noticed that his scratches were drying up and falling off. We continued administering the Ozonetherapy once a week for about 6 weeks. The improvement was dramatic!
However, one day Chance woke up with severe swelling in his left hind leg and obviously, he had difficulty walking. He received Prevacox and was stall bound for 24 hours. The vet was called and she arranged to come out the following day. The next morning, Chance’s left leg was still huge and he was having trouble putting weight on it. I did the typical leg treatments- icing, wrapping. The swelling remained. I tried to get him out of his stall to cold hose his leg and give him a bath but he would not budge. He was sweaty and breathing heavily and intermittently shivering. So, I gave him an alcohol and water sponge bath and continued to ice his back legs. I sat with him for 4 hours waiting for the vet to arrive. He had a fever and wasn’t interested in eating and his gut sounds were not as audible. He was drinking, going to the bathroom, and engaging with me. I debated giving him Banamine but did not want it to mask anything when the vet did arrive.
The vet arrived, gave him a shot of Banamine and an antihistamine and confirmed that Chance had a fever of 102 degrees and had Lymphingitis. There was no visible abrasion, puncture, or lump… I asked the vet to do x-rays to ensure that he did not have a break in his leg. The x-rays confirmed that there was no break. The vet suggested a regiment of antibiotics, steroids (I really am against using steroids due to the short-term and long-term side effects but in this case, I would try anything to make sure he was comfortable) , prevacox, and a antacid to protect Chance from stomach related issues from the medications. It was also advised to continue to cold hose or ice and keep his legs wrapped and Chance stall bound.
The following day, Chance’s legs were still swollen but his fever had broken. The vet called to say that the CBC had come back and that his WBC was about 14,00o. She suggested that we stop the steroids and do the antibiotic 2x a day and add in Banamine. I asked her if she could order Baytril (a strong antibiotic that Chance has responded well to in the past) just in case. And that is what we did.
Being as Chance had such a strong reaction to whatever it was, I did some thinking, discussing, and researching…first and foremost, why did Chance have such an extreme flare up of Lymphingitis when he was the healthiest he has ever been? And especially since he had not had a flare up in 3+ years…plus, his scratches were getting better not worse. The Ozonetherapy boosted his immune system and should provide him with a stronger defense against bacteria, virus’, etc. So why exactly was he having a flare up? And that is when it hit me!
In the past when Chance began his regiment of Transfer Factor (an all natural immune booster), he broke out in hives. The vet had come out and she felt it was due to the Transfer Factor causing his immune system to become “too strong” and so it began fighting without there being anything to fight, thus the hives. My theory- Chance started the Ozonetherapy and his body began to fight off the scratches by boosting his immune system. As the treatments continued, his immune system began to attack the scratches tenfold. This resulted in his Lymphatic system to respond, his WBC to increase, and his body temperature to spike. Makes sense…but what can I do to ensure this is not going to happen again?
My friend suggested attacking the antibiotic resistant bacteria by out smarting them…okay, that seems simple enough…we researched the optimal enviroments for the 3 types of bacteria present where Chance’s scratches are (shown in the results of a past skin scape test). The bacteria – E. Coli, pseudomonas aeruginosa and providencia Rettgeri. The literature stated that PA was commonly found in individuals with diabetes…diabetes…SUGAR! How much sugar was in Chance’s feed? I looked and Nutrina Safe Choice Senior feed is low in sugar…so that is not it. What else can we find out? The optimal temperature for all three bacteria is around 37 degrees celsius (or 98.6 degrees fahrenheit), with a pH of 7.0, and a wet environment. Okay, so, a pH of 7.0 is a neutral. Which means if the external enviroment (the hind legs)pH is thrown off, either to an acidic or alkaline pH, the bacteria will not have the optimal enviroment to continue growing and multiplying. How can I change the pH?
Vinegar! An antimicrobial and a 5% acetic acid! And…vinegar is shown to help kill mycobacteria such as drug-resistant tuberculosis and an effective way to clean produce; it is considered the fastest, safest, and more effective than the use of antibacterial soap. Legend even says that in France during the Black Plague, four thieves were able to rob the homes of those sick with the plague and not become infected. They were said to have purchased a potion made of garlic soaked in vinegar which protected them. Variants of the recipe, now called “Four Thieves Vinegar” has continued to be passed down and used for hundreds of years (Hunter, R., 1894).
I went to the store, purchased distilled vinegar and a spray bottle and headed to the farm. I cleaned his scratches and sprayed the infected areas with vinegar. I am excited to see whether our hypothesis is correct or not…I will keep you posted!
References & Information
Effect of pH on Drug Resistent Bacteriaijs-43-1-174
What does my horse’s CBC mean?

Nutrena SC Senior feed ingredience
The American Academy of Ozonetherapy
Hunter, Robert (1894). The Encyclopaedic Dictionary. Toronto: T.J. Ford. ISBN 0-665-85186-3.

Fall Fever
Today Chance had swelling of his back right fetlock. He had a fever around 104 and didn’t eat his feed. His eyes were dull and he was lethargic. He wasn’t limping but was walking slower than normal (he usually runs to the paddock or back to the barn). I decided, due to the Lymphingitis flare up on his back right leg, I would give him a shot of 5 mls (or 5 cc) of Banamine and wrap his leg. Once the medication set in, I would bring him in to give him a bath (it was 80 degrees today). So, that is what I did. By the time he was back at the barn he was covered in sweat. I cold hosed him and drenched the wrap in cool water and let him roam around the barn.
Thankfully, the vet was able to meet me at her veterinary practice so that I could pick up Baytril and more Banamine. Since Chance just had Lyme Disease (and had finished his medication less than a week ago), we are not 100% if this is a Lyme reaction or something else. The plan is to administer 25 cc of Baytril either orally, in his feed, or via IV for 6 days and Banamine 10 mls (or a 1000 lbs) twice a day for 3 days. The vet suggested that I do 5 cc of Banamine if his fever remains between 101-103 degrees and 10 cc if his fever is 103 degrees or above. During this time I will begin Prevacox- one 1/4 of a tablet once a day. After 3 days, I will discontinue the Banamine and continue the Prevacox. If his fevers are not down in two days, I will continue the Baytril but start the doxycycline as it maybe a Lyme disease symptom.
While researching Lyme Disease, I found that many people do two+ months of doxycycline instead of 30 days to ensure the disease has been erraticated completely. However, since Chance had shown such improvement after 30 days, I decided to not do another month. Maybe I should have…
However, Chance had similar symptoms when we found a small laceration in the DDFT tendon of his back left hind- swelling, Lymphingitis, fever, lethargy, no appetite, etc. If he does have an issue with his tendon I will most likely do another round of Stem Cell treatments which proved to be helpful last time. Thankfully I stored his stem cells in a Stem Cell Bank (via Vet-Stem) and can easily have them shipped.
I have a limp!
Resources on how to diagnose, treat, prevent, and handle lameness in horses
Your Horse Has a Swollen Leg – Why and What To Do | EquiMed – Horse Health Matters
Fetlock Lameness – It’s importance… | The Horse Magazine – Australia’s Leading Equestrian Magazine
Causes of Equine Lameness | EquiMed – Horse Health Matters
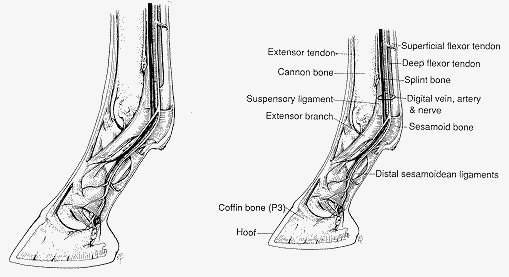
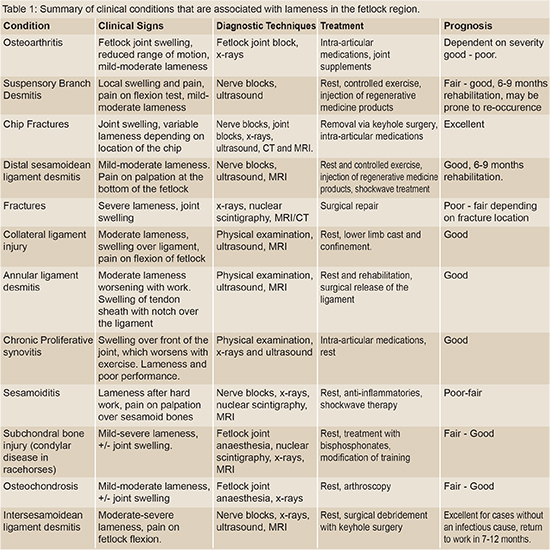
Common Causes of Lameness in the Fetlock

If You Experience Worsening Depression…
Chance began another round of Excede to get his scratches under control- it is a never ending battle. A while back, I had a skin scrape of Chance’s scratches due to their chronic nature. The scrape results showed a number of bacteria, all commonly seen with this type of infection, that were resistant to most antibiotics. Thus why we decided to try Excede.
Administering Excede is pretty straight forward- 1 shot IM every 4 days for about a month. Easy enough….or so I thought. The first shot was administered by the vet when I was not present. The second shot the vet also administered while I was there. Thirty minutes after the shot was given to Chance I noticed he seemed off but not in his “normal” post-acupuncture relaxed state. He suddenly became lethargic, he wouldn’t eat his dinner, and the gut noises became almost nonexistent. I commented to the vet my concerns and she came over and reexamined him. Sure enough something was wrong. She proceeded to administer 10cc of Banamine (just in case it was colic) and told me to walk him around outside for about 20-30 minutes. Then see if he would eat 2 cups of feed only. We walked and Chance began to act like his normal happy go lucky self. Once inside he started to eat!
Part of me felt that his reaction was a fluke. However, the third dose proved me wrong. Four days later, Chance received his shot and went outside to enjoy the first beautiful, warm day. I sat in the field watching him. He was sluggish, lethargic, stiff..he looked 10 years older and barely moved from one spot under a tree. He wasn’t eating grass nor did he run around and play- he didn’t even run up to me like he normally would. I decided to bring him inside and give him a warm bath since it was in the high 70’s. He was non responsive to his bath- no playing with the hose or even accepting peppermints. I placed a cooler on him to ensure he stayed warm until he was out in the sunshine. I figured after a bath he would perk up- again, I was wrong. At dinner time I went to bring him in and typically I will open up the gait and he will canter into his stall- he slowly walked instead. He wouldn’t eat his feed (he normally whinnies and makes a fuss until he gets his feed and devours it) or his hay…I stayed and watched him for a while and he just slept. I spoke to John, the guy who helps me with Chance and Lucky, and he confirmed that Chance hadn’t been finishing his feed and wasn’t running when he brought him in for dinner.
My concerns grew and I decided to do some research on Excede. That strange thing is I usually do extensive research before changing or administering anything with my animals. But, for some reason I did not do so this time and I wish I had.
According to a number of reputable websites, Excede can cause significant and dangerous side-effects such as; diarrhea, severe acid reflux, blood coming from mouth, loss of appetite, lethargy, muscle and gait stiffness, and more.
The most troubling of everything that I read wasn’t what was posted on the Pfizer (the manufacturer) website but from the countless statements given by horse owners and the studies done by outside companies.
According to drugs.com, “in the PK study, several horses developed clinical signs consistent with foot pain (stiff in the front limbs when turned in tight circles, and increased pulses and heat to the front feet). One horse in the NAXCEL group and one horse in the 6.0 mg/lb (2X) EXCEDE group were euthanized due to laminitis. Clinical signs of foot pain (stiff front limbs and increased heat and pulses in feet) affected more horses, for a longer period of time, in all EXCEDE-treated groups as compared to the NAXCEL-treated group. The study housing (multi-horse pens on concrete slabs) and diet (free choice alfalfa/grass mix and once a day pellets) may have contributed to the development of foot pain. The prevalence and severity of injection site reactions in EXCEDE-treated horses may also have contributed to the development of a stiff gait. A causal relationship between ceftiofur and foot pain could not be definitively determined.”
The research has revealed that Excede should be used with caution and the horse receiving the medication must be monitored. Make sure to weigh the benefits and risks before starting Excede. This drug can be lifesaving for many horses but for others, it can be life-threatening.
Excede Resources
Straight from the Horse’s Mouth: Antibiotics, Antifungals, Antivirals
Equine Product Catalog: In depth understanding of equine medications
FINALNewMexicoEIBPetitionExhibits2908-1407_pdf
CHRONIC PROGRESSIVE LYMPHEDEMA (CPL) due to Scratches
Chance has always been fighting “scratches” on his back legs. Frustrating, painful, and never seem to completely go away. Could scratches have caused this? My thoughts- scratches allowed bacteria to enter the leg, the infection settled on the DDFT sheath and caused the current flare up. Below is some research I found on possible conditions due to scratches that caused similar symptoms Chance had been experiencing.
CHRONIC PROGRESSIVE LYMPHEDEMA (CPL) due to Scratches
A condition characterized by progressive swelling, hyperkeratosis and fibrosis of distal limbs has been characterized in Shires, Clydesdales and Belgian Draft horses and unfortunately affects numerous horses within these breeds. The disease has also been recognized in Gipsy Vanners; however, only a few horses have been evaluated at this point of time. This chronic progressive disease starts at an early age, progresses throughout the life of the horse and often ends in disfigurement and disability of the legs, which inevitably leads to the horse’s premature death. The pathologic changes and clinical signs closely resemble a condition known in humans as chronic lymphedema or elephantiasis nostras verrucosa. The condition has therefore been referred to as chronic progressive lymphedema (CPL). The lower leg swelling is caused by abnormal functioning of the lymphatic system in the skin, which results in chronic lymphedema (swelling), fibrosis, decreased perfusion, a compromised immune system and subsequent secondary infections of the skin.
The clinical signs of this disease are highly variable. It is often first addressed as a marked and “therapy-resistant” pastern dermatitis (scratches). The earliest lesions, however, are characterized by skin thickening, slight crusting and possible skin folds in the pastern area. While readily palpable, these early lesions are often not appreciated visually as the heavy feathering in these breeds covers these areas. Upon clipping of the lower legs, it becomes obvious that the lesions are far more extensive than expected. Secondary infections develop very easily in these horse’s legs and usually consist of chorioptic mange and/or bacterial infections. Pigmented and non-pigmented skin of the lower legs are affected. Appropriate treatment of the infections (pastern dermatitis) is not successful as underlying poor perfusion, lymphedema and hyperkeratosis in association with the heavy feathering present perfect conditions for repetitive infections with both chorioptic mange as well as bacterial infections. Recurrent infections and inflammation will enhance the lymphedema and hence, the condition becomes more chronic. As a result, the lower leg enlargement becomes permanent and the swelling firm on palpation. More thick skin folds and large, poorly defined, firm nodules develop. The nodules may become quite large and often are described as “golf ball” or even “baseball” in size. Both skin folds and nodules first develop in the back of the pastern area. With progression, they may extend and encircle the entire lower leg. The nodules become a mechanical problem because they interfere with free movement and frequently are injured during exercise. This disease often progresses to include massive secondary infections that produce copious amounts of foul-smelling exudates, generalized illness, debilitation and even death.
TREATMENT/MANAGEMENT
Please keep in mind that none of these treatments listed below will “heal” chronic progressive lymphedema (CPL). However, a rigorous management following our suggestions below will assist you to slow down the process and even make some of the nodular lesions disappear. Your horse will need this management the rest of its life.
• Clipping of the feathers
Long and dense feathering makes management of lymphedema more difficult. We highly recommend clipping the feathers and keep them short, if horses are not presented at shows. If you have a show horse, we still recommend to clip the feathers to initiate a rigorous treatment. As the skin condition improves and the edema is reducing – you may have a better chance to keep the horse’s legs in better condition by. careful repetitive treatment, while the feathering is growing back. The feathers are usually back to their original length in about 10-12 months.
• Treatment of skin infections
Progression of lymphedema is also associated with deposition of fibrous tissue and formation of fibrotic nodules.. As a result, these horses have a poor blood circulation and immune response in the skin of their legs. They tend to built up a thick keratin layer. The long feathering further occludes the skin surface, which then remains humid. These factors provide the perfect culture environment for infectious pathogens. This explains why horses with CPL constantly battle recurrent infections with mites (Chorioptic mange) and bacterial infections (Staphylococcus, Dermatophilus).
Horses with CPL should consistently be treated against reinfestation of mites and bacteria:
Topical treatments:
• Careful washing, cleaning and drying of the legs on a routine basis is essential. Horses with long feathering may require blow-drying of their legs. We recommend using a product manufactured by HydroSurge Inc. ( http://www.hydrosurge.com ) called Apricot Sulfur Skin Treatment Shampoo.
• Frontline spray to treat chorioptic mange (do not use Frontline on pregnant and nursing mares)
• The best and most economical topical treatment is to find a source of wettable sulfur powder (“flowers of sulfur”). This can usually be found through a vineyard supply or at your local nursery (certain “rose dust” preparations). Mix this powder with mineral oil in to form a creamy paste. You can mix a moderate amount in a plastic lidded container or glass jar so that you have enough to last 2-4 weeks at a time. Apply this mixture to the ulcerated and/or affected areas of skin daily. This preparation is the best and most economical topical treatment we have found. You can use it indefinitely. Sulfur is safe to use in pregnant mares.
Systemic antiparasitic treatment: Frequent ivermectine treatment will also assist to keep the mites away.
• Exercise
Regular exercise is crucial. It will increase the circulation and the lymph drainage.
• Manual Lymph-drainage
Manual lymph-drainage is regularly used in humans with lymphedema as long as there is no inflammation present within the tissue. MLD has been successfully used in horses with more acute lymphedema, but has not been established yet in horses with progressed CPL. A massaging coldwater stream may assist a massage. It is important to dry the skin before applying anything else after massage and rinsing. If the feathers were not clipped this may take a long time and you may have to use a hair dryer. Your horse may become more compliant to this treatment as swelling reduces over time
• Bandaging and stockings
We have some limited experience with using special bandages developed for people with lymphedema. For horses, which always move around, “short-stretch” bandages should be used (example: Rosidal ®). Short stretch bandages have been successfully used in three horses with clipped feathering; but bandaging was not as successful on horses with long feathers. Of course it is crucial to have very good padding and keeping the bandages fairly tight. If tolerated, the best results will be achieved by keeping the bandages on 24/7. Of course they need to be redone at least every other day – better every day to control the legs. At first, there will be oozing from the lymphedema through the skin – so the bandages will get wet and have to be changed every day. With the reduction of the edema – this will stop. If the horse is only walked quietly the bandages can be left on for the exercise; very likely the legs have to be rewrapped after the exercise as the swelling will somewhat reduce. For more exercise it may be better to take the bandages off, use working bandages and then switch back to the short–stretch bandages after work. Again make sure the skin is dry when you rewrap.
After the edema has been reduced by using bandages – stockings are used for people to maintain avoid recurrence of lympedema. The use of such stockings in horses are currently under investigation.
It should be noted that horses suffering from CPL often are susceptible to reapeated bouts of “Thrush”. Consequently, thorough and routine foot trimming care is an essential part of the health care management for these horses.

The Call
One day I received a call that I needed to come out and see Chance because he wasn’t doing well and, according to Vet1, he needed to be put down. I quickly canceled my appointments and got on the road. The 4 hour drive was excruciating…once we finally arrived, my heart broke.
My old guy was skin and bones. His back right leg was swollen and he wasn’t able to bare weight on it. His eyes were dull. He could barely walk, and when he did, he wouldn’t put any weight on the right hind. There were even times when he would do this “neurologic dance” (coined by the farm’s owner and C’s other mom) where he would lift up his back right leg and hop!
But when he saw me pull up, he whinnied. He was excited to see me. He ate the pureed carrots but refused the apple puree (only my mom would make this for him). He wasn’t ready to die.
I called the vet who said that Chance should be put down to see what his thoughts were.
Me: What do you think is going on with C?
Vet1: I think he is ready to be put down.
Me: Because of what?
Vet1: Lymphangitis
Me: Okay, well, what is the cause of the Lymphangitis? Did you run any diagnostics?
Vet1: No
Me: I would like to manage his pain and run a few tests before making that decision. (I reviewed the research that I had done and asked where to go from there.) Could it be EPM?
Vet1: “It’s not EPM”
Me: How about Cushings? Or Laminitis? Lymes?
Vet1: Nope. Just old age.
Me: The journals I read said that some of the symptoms…(I was cut off)
Vet1: “I don’t care what journals you read! It’s a bunch of…”
Me: One was from VA Tech actually…
Well, that was that! Vet1 did not completely lack compassion but he was more “old school” I guess one could say. He was well respected in the horse world and up until this point, he did the job I needed. But I will say I was disheartened by our conversation.
I decided to contact the other vets that I had worked with in the past, who also knew Chance, and get second, third, fourth opinions.




